Tendonitis, Tendon Pain and Tendinopathy
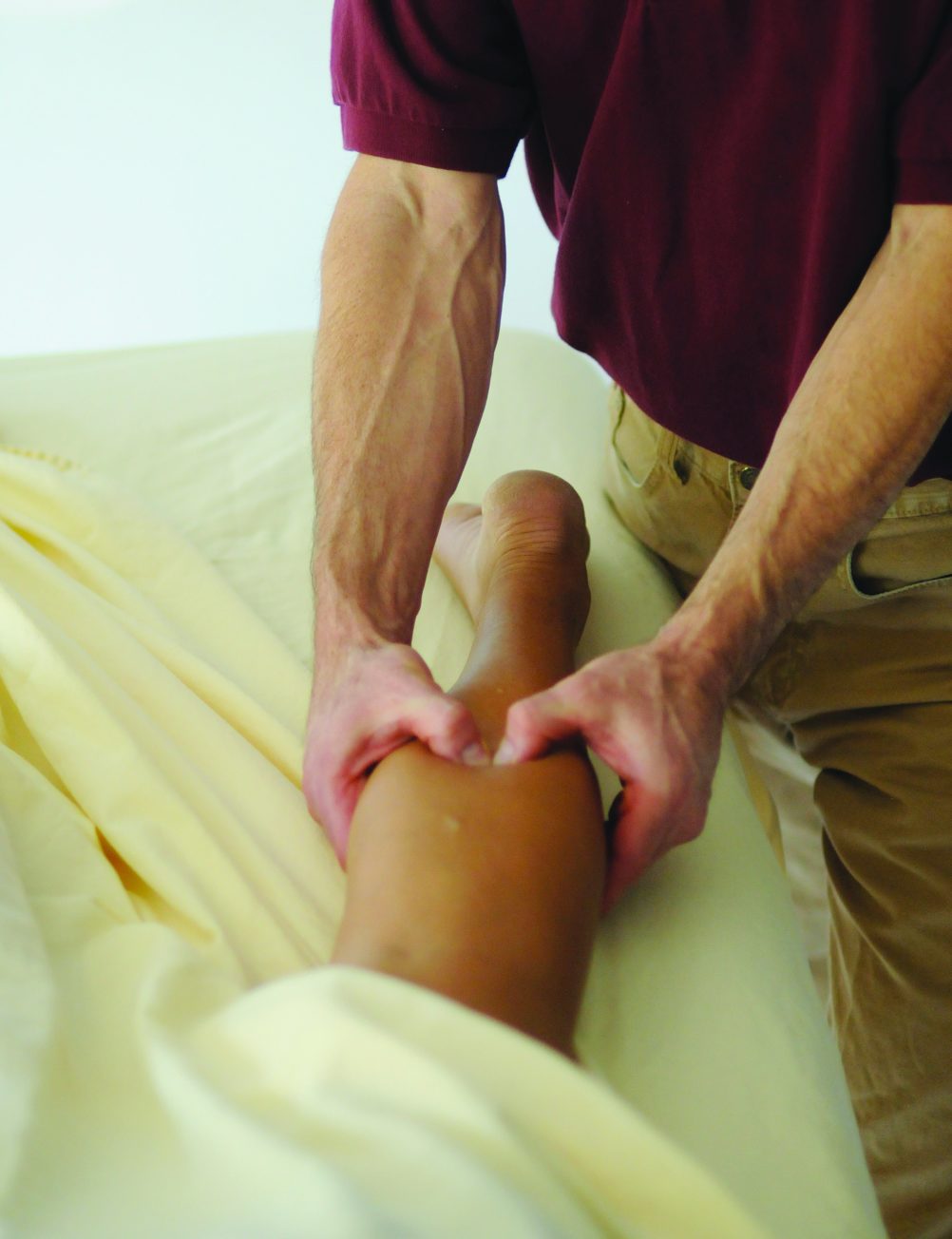
 Tendons attach muscles to bone. They are all over the body but there are a few tendons, such as the neck, elbows, biceps, wrists and achilles, which can have a condition called tendonitis (also called tendinitis) or tendinopathy. When left untreated, these areas can progress into calcific tendonitis, a condition that is usually considered irreversible and alleviated with corticosteroid injections or in severe cases surgery.
Tendons attach muscles to bone. They are all over the body but there are a few tendons, such as the neck, elbows, biceps, wrists and achilles, which can have a condition called tendonitis (also called tendinitis) or tendinopathy. When left untreated, these areas can progress into calcific tendonitis, a condition that is usually considered irreversible and alleviated with corticosteroid injections or in severe cases surgery.
After decades of soft tissue practice, we have found that tendonitis also occurs in the back muscles. “Chronic tendon pathology is a common and often disabling condition, the causes of which remain poorly understood” (McCreesh & Lewis, 2013). In many cases, loss of concentration and the ability to perform daily or work tasks result. Depending on the situation and person, worry and depression can also occur.
Why do Tendons Calcify?
The physiological process of how the tendons calcify is not known in it’s entirety but it is being studied. Small micro tears form in the tendon from overuse, misalignment or injury. Silverthorn (2016), describes tendons as dense connective tissue made of collagen that do not stretch and connect muscle to bone.
Tension is placed upon tendons during movement and constantly placed upon them during misalignment, excess tightness, weakness or compensation patterns and poor posture. Collagen fibers are laid down in parallel strips and when strained, overused or compressed they can tear, fray and get inflamed. This can be an acute or chronic issue.
Calcific Tendonitis and the Matrix Vesicles
“Calcific tendonitis is associated with tendon rupture pro long symptoms of pain and lack of range of motion discomfort and stiffness and poor response to Physical therapy” (Golub, 2009). The current continuum model of tendon pathology is that if left untreated calcification occurs. This is a continual and prolonged process of complexity.
McCreesh and Lawrence imply that early stages of tendonitis is called reactive proliferation tissue reaction where the tendon thickens due to the up regulation of large proteoglycans and an increase bound of water. The second level is despair and characterized by greater colleges separation and abnormal tendon cycles as well as an increase in neovascularity. These two stages have some degree of reversibility within the appropriate healing environment. When not healed, the tendons move onto stage three where calcium gets laid down by matrix vesicles . These microscopic vesicles drill out a pathway into collagen where calcium is subsequently laid down.
“Tendon calcification is generated by extra cellular organelles, called matrix vesicles, which are small 20-200 no spherical bodies observed in the pre-mineralized matrix of cartilage surrounded by a lipid layer and forms crystals” (Golub, 2009). The process of calcification eliminates some or most of the inflammation and in some cases the tenderness but it creates an area prone for soreness, stiffness and tightness, achiness and predisposition for injury. In many cases, there is a visible deformity. Often we see this in the back, when the muscles becomes bowed.
Effects of Tendonitis
As the condition develops, it has great impact on our homeostasis, both physiologically and psychologically. “The process at the cellular level is now more understood that thinking and feeling influence homeostatic control via autonomic endocrine in immune output systems” ( Henderson, 2005). The more it hurts, the more we worry and the more we worry the more it hurts. We stay in the feedback loop that is not healthy.
The three stages to notice are inflammatory, regenerative (when it seems to be less painful, but really the body is adapting) and degenerative when the calcification is set in. This can be permanent if not stopped early enough. In many cases, improvement is seen when addressed properly. The process of ignoring, squeezing, randomly rubbing or trying to workout harder is not very effective. Neither is medicating the mind or the inflamed area. “Problems with weakness and improper posture or work habits tend to worsen as the day progresses and fatigue sets in” ( Riggs, 2007).
Treatments for Tendonitis and Tendon Pain
Appropriate therapy such as ice, cross friction massage, stretching, properly aligned strengthening programs and the use of Arnica gel twice/day for 21 days has shown in studies to be effective (daSilva et al., 2015). If appropriate therapies are not administered soon enough or long enough, then the area can fall into a negative feedback loop.
Silverthorn states that “A System that reinforces the stimulus is not homeostatic and will need an outside intervention in order to stop.” “Tendons respond well to massage and ice” (Riggs, 2007). And when outside intervention is not applied effectively, the negative feedback continues over time, months and even years, and calcification develops. Tendons become less supple, swollen, tender and stiff causing reduced range of motion and pain.
Proper and guided stretching and strengthening can help. So can the use of acupuncture to reduce inflammation. Proper and adequately applied massage techniques along with rest and biomechanical retraining often produces results. Ice and the use of KT or athletic tape may also be effective. All of these modalities are available at Boulder Therapeutics.
———————————
Thanks to our massage therapist, Rene, for her contribution to this article.